Detroit Street Care: Student-Led Medical Outreach
- Allison Jennens
- President, Detroit Street Care
- College of Osteopathic Medicine
- Jaclyn Israel
- Communications Coordinator, Detroit Street Care
- College of Osteopathic Medicine
- Dean Carpenter
- Family Nurse Practitioner
- Neighborhood Services Organization
- Richard Bryce
- Faculty Advisor, Detroit Street Care
- Assistant Professor, College of Osteopathic Medicine and Wayne State University
- Chief Medical Officer, Community Health and Social Services, Detroit

Allison Jennens and Jaclyn Israel saddle up for a street run.
The Tumaini Center is a crisis support hub at Mack and 3rd Avenue that is run by Detroit's Neighborhood Services Organization (NSO). Tumaini is the last stop even for regular shelter-goers. It is the only shelter in Detroit open 24-7. Its clients include those with behavioral issues severe enough to get them turned away from other shelters. Services are beyond bare-bones: There are no beds—not even cots—only a couple of large rooms filled with battered metal folding chairs where people experiencing homelessness can come in to sleep. But hot coffee is available, along with laundry facilities, showers, and a friendly welcome for everybody.
Before 2012 the Tumaini Center's medical service consisted of a part-time staff of one: Dean Carpenter, a family nurse practitioner who also worked at the University of Michigan Health System in Ann Arbor, who came in for two days a week. That was about enough time to handle the most urgent cases, but nothing else.
.jpg)
MSU physician Richard Bryce works with Detroit Street Care, an organization that provides medical care to those in need in Detroit.
Student-Based, Health-Professional-Led, and Patient-Centered
Then, Jonathan Wong, a medical student at Wayne State University, was inspired to found a clinic that would serve Detroit's homeless community (at the time nearly 20,000 people) directly on the streets and in shelters. Thus, in 2012, with the support of Wong's medical school colleagues and the NSO, a new student organization at Wayne State was born: Street Medicine Detroit (SMD), which billed itself as "student-based, health-professional-led, and patient-centered."
Two years later the fledgling organization was ready to take on new partners. MSU was a natural. Its College of Osteopathic Medicine has a branch campus at the Detroit Medical Center and a strong commitment to public health. Also, both Carpenter and the new medical director of Wayne's Street Medicine Detroit program, Richard Bryce, had received their degrees from Michigan State.
Carpenter had already moved to the NSO full-time when Bryce took on the MSU Detroit Street Care directorship in 2014 (in addition to his faculty appointments at MSU and Wayne; he is also chief medical officer at Community Health and Social Services, a community-based nonprofit that provides health care and support services in partnership with the Henry Ford Health System).
Two Programs Working in Tandem
The MSU and Wayne State teams run separate operations, but with a common goal. They work side-by-side to cover different days and shelters to ensure the clinic is open as often as possible. They share resources—such as a joint EMR—that allow them to provide more thorough and continuous care to some of their regular patients, even when they're not working directly with each other.
The two teams also collaborate on health fairs and community events in Detroit that they are invited to. For example, Councilwoman Pro Tem Mary Sheffield hosts an annual event called "Occupy the Corner" and the two schools staff a table at the event, talking about street medicine and doing blood pressure screenings. This year they co-hosted a table at the NAACP conference, held in Detroit, in July.
A Day at the Clinic

Jaclyn Israel checks supplies at the Tumaini Center clinic.
On MSU's day at the Tumaini Center clinic there will usually be 4-10 students. MSU-COM overall has about 100-200 volunteers for the program every year. Although there are only 50 students per class at the Detroit campus, the interest and passion for street medicine has grown so much that students from all three campus locations are now participating. In turn, DSC supports a sister operation in Lansing called Spartan Street Care.
Allison Jennens and Jaclyn Israel are two second-year Osteopathic Medicine students at MSU. Jennens is president of the Detroit Street Care team and Israel is its communications coordinator.
There is no dedicated clinic space at the Tumaini Center. Jennens, Israel, and their colleagues see patients in a small conference room, all squeezing around each other as necessary. In another room there is a cabinet with medical supplies (many of them donated) and a small, curtained-off area where they can do private examinations. If the clinic is not too busy, it might be possible to find a quiet corner for a doctor and/or social worker to talk with a patient about personal challenges and whether resources are available to help.
Jennens said they treat the most common and acute ailments related to homelessness—things like boxer's fracture (broken knuckles), stasis ulcers (treated with Unna boots), and pneumonia ("most patients are smokers"). Another common complaint is fluid in the legs (peripheral edema). Unfortunately, this condition is exacerbated by sleeping upright in chairs.
Bryce pointed out that the Detroit Medical Center campus is only a mile away: "It's beautiful. But between here and there you walk by places you have no idea people are living homeless. If you forget, they're still here. Everything for them is complicated."
In addition to their work at the clinic, the students go out on weekly street runs, looking under bridges and in alleys for anyone who might not make it through the night. A van drives them out to several drop-off points in groups of five (mixed juniors and seniors), or they go out on bicycles, carrying medical kits in their backpacks, along with socks, gloves, and other supplies. Again, the Wayne and MSU teams usually go out on different days to reach more people, but sometimes if there is a specific need they will pool their resources to handle it. For example, during the spell of polar vortex weather last winter, they all went out with blankets, clothing, hot chocolate, soup, offers of a ride to the nearest shelter, and anything else they could think of to help.
"The Students Help Decide What We Do"
The MSU program is student-led. This means that with guidance from Bryce and Carpenter, Jennens and her crew take on the challenges of funding, resourcing (not necessarily the same as funding), programming, partnership-building, and other administrative functions while attending to their medical education. Bryce said, "The students help decide what we do. When ideas come up, they set up the training, get the medications paid for, and disperse them in the community."
Funding issues are never-ending. The Detroit Medical Center was recently purchased by a for-profit corporation that does not plan to continue the hospital's support for the Street Care operation. Israel wonders whether its new owners will notice that "the days this place is open, the number of ER calls drops. In the City of Detroit in 2017, NSO made the most 911 calls, right from here. But when the clinic was open, 90% of the 911 calls came in on days no students were here. It's hard to get funded if you don't add any new services, just reduce the ones the city has to respond to. You're invisible."
They are canny about finding resources and partners. For example, Israel said, "We were asked by Detroit city health services to address the Hepatitis A epidemic. The Centers for Disease Control helped us get a refrigerator certified to store the medications."
Last year Troy Athens High School chose Detroit Street Care as the beneficiary of its annual charity drive and came up with a stunning $148,000 donation—but even that was a one-time windfall. According to Carpenter, the NSO is trying to come up with more stable funding through community grants and partnerships.
Taking on Opioid Addiction
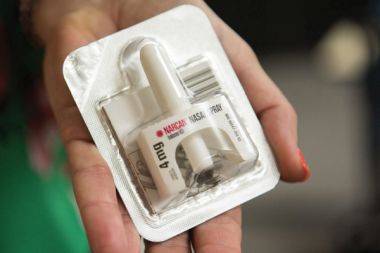
Narcan® nasal spray is freely available from any pharmacist, without a doctor's prescription.
The biggest issue the Street Care team is struggling with right now is the opioid addiction epidemic that is sweeping the country.
"It can be anyone," said Bryce. "We all hear about it and know it's a problem, but we like to think of it as being at one remove. What do you do when somebody overdoses in your space? It affects everyone. This is a change that's happened across the country."
The team is developing a program to disseminate NARCAN® kits and train community members in how to use them.
NARCAN® (naloxone) is used for the complete or partial reversal of overdose. Its effects begin within 2-5 minutes after the medication is administered. Anyone can purchase NARCAN® Nasal Spray directly from a pharmacist, without a doctor's prescription. Injectable varieties and multiple-dose kits require a bit of medical training to administer.
The drug has proved to be something of a silver bullet, with a high success rate. The catch is, time is of the essence; also, multiple doses may be required. But, given its proven ability to save lives, "There's no excuse for not having access or not knowing how to use it," said Bryce.
Earlier this year, a woman collapsed by the door just as a street team was headed out to a soup kitchen. One of the students started rescue breathing and Carpenter administered NARCAN®. "One dose didn't work but the second one did. This happens quite a lot," said Israel.
In another case, said Carpenter, "A guy was sleeping in the corner of the men's section where there are some cots for sick people. The desk came over and said somebody's out. We gave him NARCAN® and he woke up." After that, the team put a phone number in the street-run kits and "NARCAN® available" signs in the bathrooms.

Dean Carpenter is a nurse practitioner who ran the Tumaini Center clinic as a staff of one before 2012, when the first student-led program came on board.
They started a training program for community members who want to learn how to use the kits, and joined them for the training to see what kinds of issues came up. "That was valuable," said Israel.
"It's an incredible program," said Bryce. "It's awesome because it comes from the students. Allison and Jaclyn will pass it on to the next group. It's just the beginning."
Their first priority was to get more kits. Using the Troy Athens money, they funded the initial inventory themselves, and also reached out to Families Against Narcotics and other partners. They now have some kits for front desk supplies and a few more they have been dispensing to street partners.
Carpenter said they are "pretty picky" about who gets the treatment kits: "We gave one to a guy who was off drugs but had just lost an addict friend. We gave him the training and a kit."
They are beginning to connect with other organizations that are tackling the same issues. Jennens and Israel have met with staff at Covenant Health (an organization that works with street sex workers), Families Against Narcotics, Hope Not Handcuffs (which provides an addiction rehab program), and other groups. They are also working with the state police.
A New Area of Research and Practice
Street medicine is fast becoming a new area of medical research and practice, and Jennens and Israel are excited to be on the frontline. "We went to an international street medicine symposium in the Netherlands," said Jennens. "We learned all sorts of stuff. Some groups even have a treatment bus. They're doing safe needle exchange, recovery day houses… Having regular activities and a place to be, they show better results."
At the Tumaini Center, new partners are coming on board. NSO is building relationships with the universities. The NARCAN® program is growing. Street care is now available as a fourth-year elective at MSU-COM. "Nobody else does that," said Carpenter.
Still, none of this solves the pervasive problems of poverty and injustice in the world, the results of which the Detroit Street Care team confront daily, with remarkable courage and resourcefulness. "We know we can't fix their lives," said Jennens. "Our goal is to provide access to the healthcare they need, and treatment for their ongoing issues, so that they can have hope for the future."
- Written by Linda Chapel Jackson, University Outreach and Engagement
- Photographs courtesy of University Communications, Nick Hagen, Bonnie Arbittier (@Flickr) and Paul Phipps, University Outreach and Engagement